Background
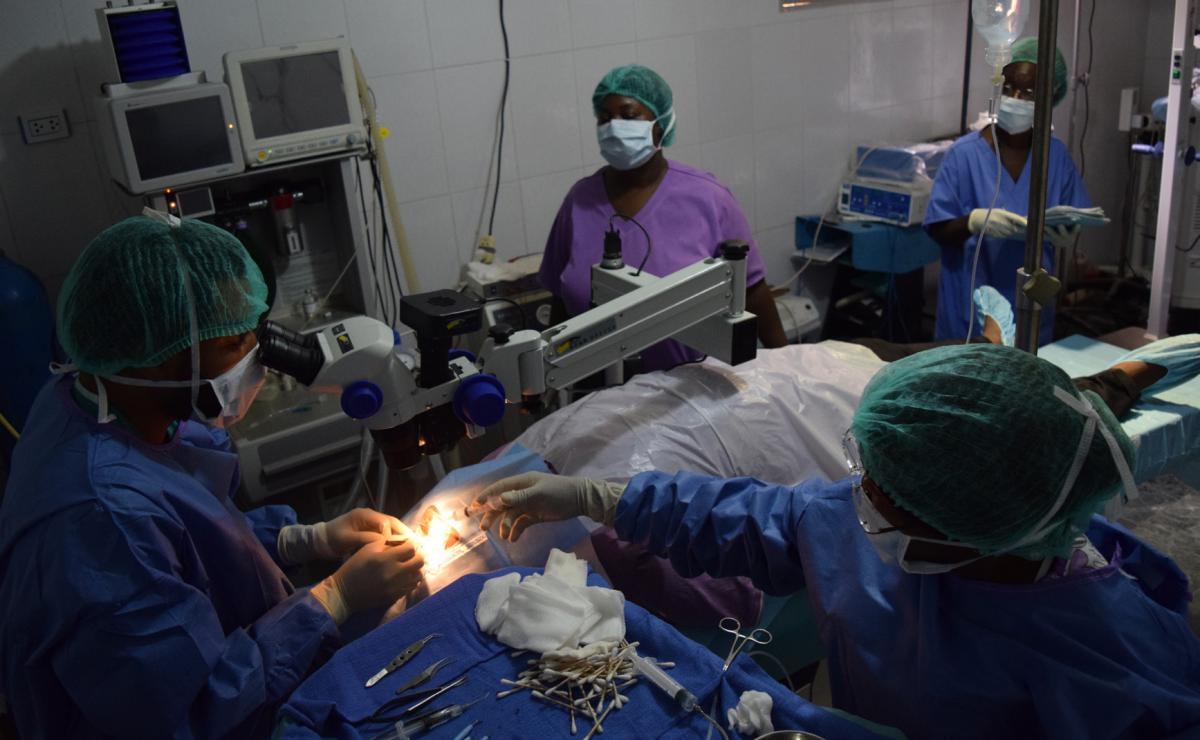
Dr. Udofia conducting surgery on a patient.
While Liberia’s 2014-2015 Ebola epidemic has passed, the challenges rebuilding the public health system and addressing system constraints persist. In addition, many survivors exhibit a range of ophthalmic, psychiatric, and rheumatologic conditions, including uveitis, post-traumatic stress disorder, and arthralgia. Although they had access to basic health services and generalists, clinical specialists and advanced services were limited, especially to those living outside of Montserrado county.
In 2017, the USAID-funded Ebola Transmission Prevention & Survivor Services program (ETP&SS) selected the Liberia College of Physicians and Surgeons (LCPS), a graduate medical residency program that supports advanced training for physicians across a range of medical specialties, to independently manage the complex medical and surgical cases of Ebola survivors, as well as to offer specialty care to the general population. Historically, LCPS has recruited clinicians from the West Africa sub-region (and beyond) to train Liberian clinicians and medical students in a range of specialties.
Through a grant provided by ETP&SS, LCPS recruited four clinical specialists for long-term postings in Liberia to provide specialty care in ophthalmology, mental health, psychiatry, and rheumatology, and to build the capacity of local medical personnel to provide these services and to refer cases that they cannot manage. While the grant emphasized the Ebola virus disease (EVD) survivor population, three of the specialists offered their services to the general population as well.
Intervention
The LCPS program started in June 2017 with LCPS and ETP&SS staff jointly recruiting the four clinical specialists for ten month consultancies. The specialists provided training and clinical services at several ETP&SS focus hospitals, including Redemption Hospital and John F. Kennedy Medical Center in Montserrado County; Phebe Hospital in Bong County; and Tellewoyan and Foya Boma Hospitals in Lofa County. “You find 95 percent of EVD survivors in these areas,” explains the Clinical Specialist Program Coordinator, Dr. Isabel Simbeye. Targeting and reaching survivors in high-concentration EVD survivor communities ensures that the services are fully utilized by survivors.
The Clinical Specialist program staff was comprised of four specialists: two psychiatrists, a rheumatologist, and an ophthalmologist. Dr. Simbeye emphasized, “We’ve never had a rheumatologist in Liberia before. Through funding from USAID, ETP&SS also provided basic equipment and actively worked to build the capacity of health workers in these facilities so that even after the program phases out, knowledge transfer will have occurred and services can continue.”
LCPS’ M&E Officer, Robert Hiama noted “I go to the clinics to see what services are being provided. I talk with patients to find out if those services are what they need, and if they have problems. Then Dr. Simbeye and I discuss and resolve the problems, such as survivors not receiving drugs or services, and feeling like they aren’t being respected by the health workers.” Mr. Hiama further explained, “The specialists collect data through the patient register, which was jointly designed by LCPS and ETP&SS M&E staff. There’s also a feedback monitoring tool, which we use to collect feedback from survivors on the services they are receiving.” Mr. Hiama noticed improvements in the ability of patients to explain issues to doctors, as well as interpersonal dynamics between the survivor and providers.
Dr. Musa Gambo Takai, one of the program’s two psychiatrists, provided mental health services to EVD survivors and the general population through counseling, treatment, and medications. He also trained and mentored mental health clinicians, physician assistants, nursing students, and physicians in the diagnosis and treatment of common psychiatric and neurological conditions, such as depression, and anxiety and post-traumatic stress disorders. “We’ve accomplished a lot and have seen an increased awareness in communities around mental health and treatment, and reduction in stigma attached to mental illnesses, resulting in improved services for survivors. The more people are enlightened about mental health, the more comfortable they will be accessing or reaching out for these services,” he explained.
Outcomes
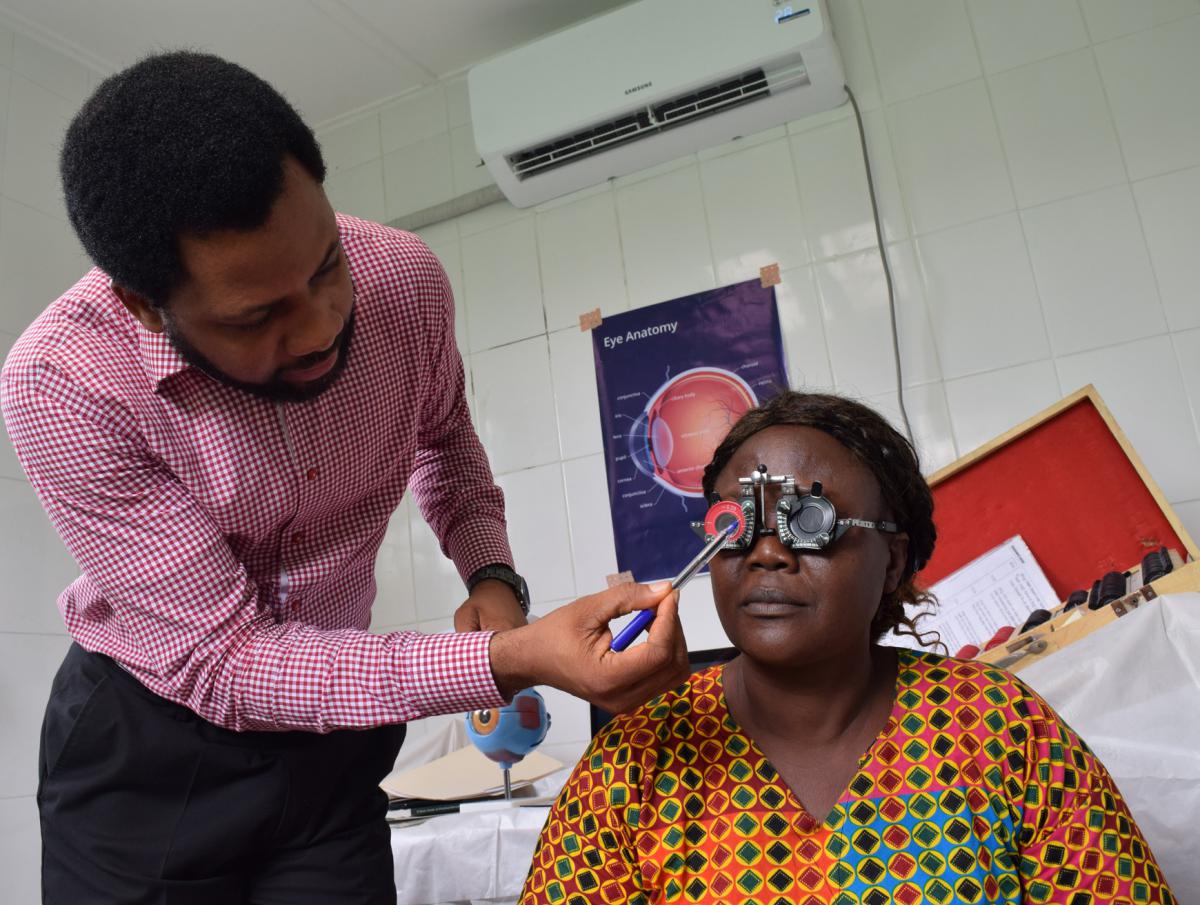
Dr. Udofia leading a training on ophthalmic care.
Dr. Inyene Edem Udofia, the LCPS ophthalmologist, noted that “before, no facility provided eye care in the entire county. We’ve recruited and started training health workers.” Thus far, one physician assistant and six nurses registered for the ophthalmic care program, which focuses on retraining health workers with prior ophthalmic training to update their knowledge and skills. Dr. Udofia believes that although ophthalmology is still a relatively new field in Liberia, he is optimistic that the increased availability of trained medical professionals will strengthen eye care service delivery in Liberia. “I’ve worked with nurses who are very enthusiastic and have a passion to learn. They are trained in basic eye care, including eye-related emergencies. And we’ve trained them to train junior nurses and community health workers.” By training health care workers and educating communities on basic eye care services, Dr. Udofia is confident that eye care services will continue to be delivered even after the ETP&SS program ends. Similarly, Dr. Takai expressed, “If the health workers who’ve been trained maintain the interest and motivation, they’ll be able to do well.” And the Liberian people—EVD survivors or not—will do well under their care.






